When you face many damaged or missing teeth, you carry more than a smile problem. You carry pain, strain, and worry every day. Full mouth restoration can stop that cycle. It starts with careful planning, not guesswork. An implant dentist studies how you chew, speak, and smile. Then the dentist designs a step‑by‑step plan that fits your mouth, your health, and your daily life. You see clear goals, clear timing, and clear costs. This blog explains how implant dentists map out your new bite, choose each implant position, and match tooth shape and color. It also shows how your medical history, bone strength, and jaw movement guide every choice. If you need oral surgery in New Braunfels, TX, this same planning process protects you. You deserve a calm, steady path to a mouth that feels strong, looks natural, and works every single day.
Step 1: Listening to Your Story and Goals
Planning starts with you. The dentist asks about your pain, your daily habits, and your hopes.
You may talk about:
- Teeth you avoid chewing on
- Food you cannot eat now
- Jaw or head pain
- Past dental fear or hard visits
The dentist also reviews your medical history. This can include heart disease, diabetes, tobacco use, and common medicines. The National Institute of Dental and Craniofacial Research explains that these health factors change how implants heal. Clear talk about your health lets the dentist plan safe care.
Step 2: Detailed Exam and Scans
Next, the dentist studies your mouth in three ways. You feel seen from every angle.
- Clinical exam. The dentist checks your teeth, gums, bite, and jaw joints.
- Pictures and models. Photos and digital scans record how your teeth look now.
- 3D imaging. A cone beam CT scan shows your bone height, width, and nerve paths.
This information shows which teeth can stay, which should come out, and where implants can sit. It also shows how much bone support you have. If the bone is thin, the dentist may plan bone grafts first. That step can prevent implant failure and repeat surgery.
Step 3: Building Your Custom Treatment Map
With your story and your scans, the dentist builds a clear plan. You see a sequence, not a guess.
The plan often covers three main stages:
- Getting your mouth healthy
- Placing implants
- Attaching new teeth
The dentist explains what happens in each stage. You hear how many visits you need, how long healing may take, and what you can eat at each point. This removes fear. It also helps you plan time off work and family support.
Step 4: Choosing the Right Type of Full Mouth Restoration
Not every person needs the same kind of full mouth restoration. The dentist weighs your health, bone strength, and budget. Then you choose together.
Common Full Mouth Options With Implants
| Option | Implants Needed | Removable or Fixed | Typical Benefits | Points to Consider |
|---|---|---|---|---|
| Implant supported denture | 2 to 4 per jaw | Removable by you | More stable than a regular denture. Easier speech and chewing. | Still removed for cleaning. Bulkier than fixed teeth. |
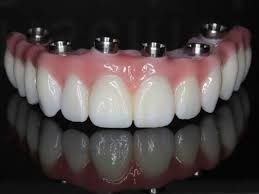
| All on 4 style fixed bridge | 4 to 6 per jaw | Fixed. Removed only by a dentist | Strong bite. Slim design. Feels close to natural teeth. | Harder cleaning under the bridge. Needs good bone in key spots. |
| Individual crowns on many implants | 8 or more per jaw | Fixed | Each tooth stands alone. Natural look and feel. | More surgery. Higher cost. Longer timeline. |
This chart is a guide. Your dentist tailors it to your mouth and your goals.
Step 5: Digital Design of Your New Smile and Bite
Next, the dentist designs your future teeth on a computer. You may see a digital mockup of your new smile.
The dentist chooses:
- Tooth length and width
- Tooth color
- How your upper and lower teeth meet
This design protects your jaw joints and neck. A poor bite can trigger pain and broken teeth. Careful design spreads chewing force across your implants. That keeps them steady for many years.
Step 6: Surgical Planning That Puts Safety First
Now the dentist plans the exact implant positions. The 3D scan and digital design guide every move.
Many dentists use a surgical guide. This is a custom template that fits over your gums. It marks where the implants go. This guide helps protect nerves and nearby teeth. It also helps the dentist place each implant at the right angle.
The Centers for Disease Control and Prevention describe how gum disease can damage bone. If you have gum disease, the dentist treats it before or during implant care. Clean, stable gums give your implants a stronger base.
Step 7: Temporary Teeth and Healing Time
During healing, you still need to speak and eat.
Your plan may include:
- Immediate temporary teeth on the same day
- A removable denture while implants heal
- Soft food rules to protect new implants
These steps protect your implants from too much force. They also give you a smile in social settings while bone grows around the implants.
Step 8: Final Teeth and Long Term Care Plan
After healing, the dentist attaches your final bridge or crowns. You test your bite. You share what feels off. The dentist makes small changes so chewing feels steady and pain-free.
You also get a long-term care plan. This often includes:
- Regular cleanings and exams
- X rays at set times
- Night guard if you grind your teeth
- Home care steps with brushes and floss tools made for implants
Routine care keeps your gums healthy and your implants stable. It also lets the dentist catch small cracks or loose parts before they break.
How to Use This Planning Process for Yourself
You deserve a clear plan, not rushed treatment. When you meet an implant dentist, ask three questions.
- How will you study my bite, bone, and medical history
- What are my full mouth options, and why do you suggest one over another
- What will my month-by-month plan look like
Careful answers show respect for your body and your time. With a strong plan, full mouth restoration becomes less scary. You move from daily strain to steady function. You protect your health, your speech, and your confidence with each step.